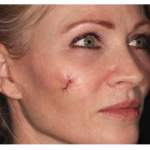
Technique of Reconstruction
Technique of Reconstruction
Home > Reconstruction > Technique of Reconstruction
SKIN RECONSTRUCTION OVERVIEW
Skin cancer excision creates a tissue defect that may require surgical repair. Each of the many reconstructive techniques is used for different types of skin cancer defects. The surgical repair can be done by the Mohs dermatologist or may require reconstruction by a plastic surgeon. Certain defects do not require surgical repair at all as the body heals itself. Careful planning is necessary to achieve great results and to avoid problems.
LINEAR CLOSURE
This is the most straightforward technique of closure of a skin defect. It usually requires additional resection of skin, beyond the necessary margins of excision of a lesion. The resection of skin is done to change the defect shape from a round or an oval into a fusiform shape that can be closed as a line. Sutures are used to bring the deep tissue layers together first, followed by more superficial layers of the skin. Traditional external sutures over the line of closure can be used as a final layer. Sometimes, only internal sutures are required to bring the wound edges together.
LOCAL FLAPS
When tissue is removed surgically from the face, such as in skin cancer removal, an open wound (or defect) remains. Reconstruction (or closure) of the defect may be done using a local skin flap.
ISLAND FLAPS
An island flap is created by using the adjacent healthy tissue to repair a defect. It is the workhorse flap of advanced skin cancer reconstruction. The island flap is usually triangular or a tear-drop shape. Its hallmark is avoidance of additional skin excision and even distribution of repair tension. The island flap uses fewer incisions and creates less scarring than local skin flaps.
REGIONAL FLAPS
A regional flap is similar to an island flap, but is used when a much larger section of tissue is required. Very invasive or advanced skin cancers on the nose can result in deep and large nasal defects. This requires major nasal restoration and several stages to repair. The technique which has been most reliable in this type of repair is the regional flap. All three layers of the nose (the cutaneous outer skin, the structural support, and the inner lining) may need to be replaced. A section of tissue, including the deeper layers, is partially released from either the forehead or the nasolabial area of the cheek while the area proximal (closest) to the defect remains temporarily attached to the body’s vascular supply. It is then used to replace the large area of missing tissue while retaining its vital blood supply.
SKIN GRAFTS
When tissue is removed surgically from the face, as is done in skin cancer removal, an open wound (or defect) remains. Reconstruction (or closure)
of the defect may be done using many techniques, depending on it’s size, depth, location and surrounding skin type. If the defect is superficial and in an area of tension, such as the nose, a skin graft may be used to complete the reconstruction.
CARTILAGE GRAFTS
When a skin cancer is removed from the ear or nose, the remaining defect may be deep enough to involve the cartilage below. Cartilage is the stiff, supporting structure which creates the shape of the outer ear and nose. When a portion of this cartilage is removed, it often needs to be replaced in order for the structure to maintain its previous shape.
COMPLEX MULTI-FLAP RECONSTRUCTION
Some of the more invasive or advanced skin cancers result in defects which may require complex multi-flap reconstructions. A complex defect is determined by size, lack of structural integrity due to missing mucosal lining, cartilage, fat and muscle, or small defects on the nose or eyelid where simple closures will leave aesthetically displeasing results.
POLY-DIOXANONE (PDS) PLATE FOR RECONSTRUCTION
PDS (poly-dioxanone) absorbable plates (Ethicon) have recently been approved by the FDA for septal and nasal reconstruction.
SECONDARY INTENTION HEALING
When tissue is removed surgically from the face, such as in skin cancer removal, an open wound (defect) remains. If the defect is very small and superficial, there may be an option to let the wound heal on its own, rather than having it surgically repaired. This natural healing of defects is called secondary intention healing. It may be a good choice for patients who are poor surgical candidates or who are not concerned with an optimal cosmetic outcome. Sometimes, secondary intention healing can actually produce superior cosmetic results. Experienced reconstructive surgeon can help the patient make that decision.
FREE FLAPS
There are circumstances when a large area of tissue on the face is damaged or surgically removed. Some possible causes are cancer removal, immune and inflammatory diseases, radiation, and trauma. Reconstruction of these defects is challenging and requires a free tissue flap.
PROSTHETIC EAR RECONSTRUCTION
When skin cancer involves a large portion of the auricle, surgical treatment options include either Mohs excision or subtotal or total resection of the auricle. Each surgical approach has its unique advantages. Prosthetic reconstruction of the auricle offers the aesthetic rehabilitation option that can change the surgical treatment approach to skin cancer of the auricle.
SCARS FOUNDATION
COORDINATE CARE WITH SCARS
PRESENT A SKIN CANCER CASE
STAY UP TO DATE
Receive research updates, inspiring stories, healthy living tips and more.
!
!
SUBSCRIBE
Something went wrong. Please check your entries and try again.
Education
Selected Stores
Coupon Deals
FashionFreaks VIP
Currency Converter
Popular Outlet Stores
Research
Your Account
Renew Subscription
Member Deals
Get VIP Account
Recommend a Friend
Treatment
Contact FF
Magazine Authors
Press Center
Careers at FF
Terms & Conditions
CME ACCREDITED SKIN CANCER CONFERENCE
Earn your 2018 CME credits at the SCARS Foundation Monthly Skin Cancer Conference
FOLLOW US
ELEVATING THE STANDARDS OF SKIN CANCER MANAGEMENT.
© 2017 SCARS Management Services. All rights reserved.