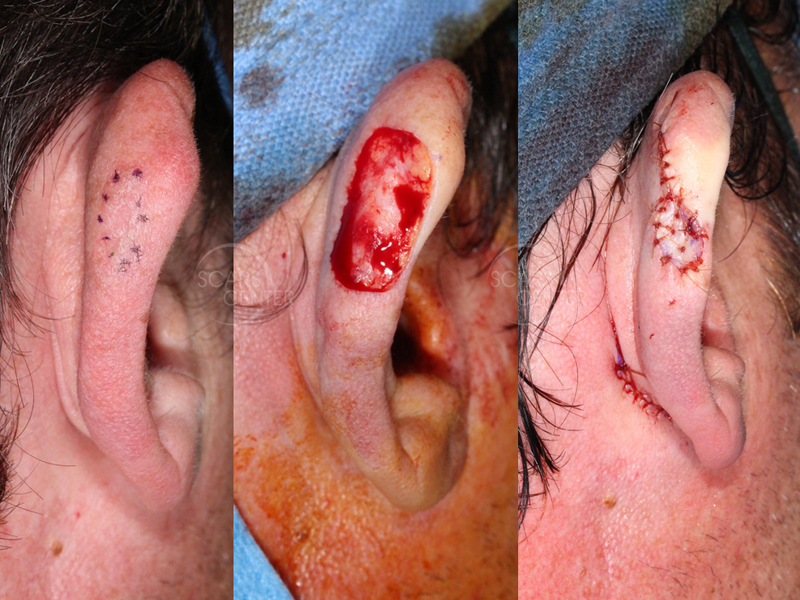
Right Ear Melanoma In Situ with Depth Uncertainty – The role of Histopathologic Discordance in Clinical Decision Making
HISTORY
40-year-old man presents with a 2 month history of right posterior ear pigmented papule. Shave biopsy on 9-18-17 showed malignant melanoma at least in situ. Excision with 5 mm margins on 10-9-17 confirmed residual melanoma at least in situ with clear margins.
DISCUSSION
Lack of superficial invasion cannot be definitely ruled out after a superficial shave excision of a melanoma. Pathologists are left to interpret whether the intradermal nests of atypical melanocytes are part of the extension along the basement membrane into the dermal appendages, or whether these intradermal nests represent superficial dermal invasion. In cases of superficial dermal invasion that would be confused with dermal appendage extension of atypical melanocytes, the invasion depth is normally no more than 0.2 – 0.3 mm. In our case, this distinction could not be made even with additional wide local excision. But is this distinction between melanoma in situ and and early invasive melanoma important? Is a minimally invasive melanoma different from a presumed melanoma in situ? Can the two diagnoses be made with 100% certainty?
The last question can be clearly answered as no. There is significant discordance in histopathologic diagnosis of melanocytic lesions. Therefore, a lesion defined as a melanoma in situ can in fact be an invasive melanoma and vice versa. There are multiple studies showing significant diagnostic discordance even among expert referral center pathologists. The rate of melanocytic lesion histopathologic discordance is anywhere from 4% to 30%. These differences would impact the clinical management of the patients.
So, the difference of 0.2 mm of invasive melanoma vs a melanoma in situ may be purely academic. The treatment would remain the same. It is appropriate to expect the histopathologist to seek multiple intradepartmental consultations or even additional outside opinions.