Upper Chest BCC PNI
HISTORY
53-year-old man presents with a 4-year-history of BCC of upper chest. The tumor measured 12 cm x 6 cm. Wide local excision with 1 cm margins on 11/10/2017 found clear margins and perineural invasion. The nerves up to 0.23 mm were involved by tumor. The final defect was 13.5 cm x 8.3 cm.
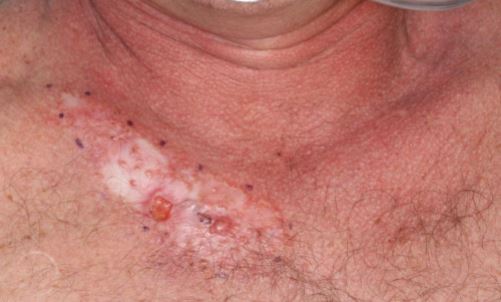
12 x 6 cm basal cell carcinoma of the upper chest.
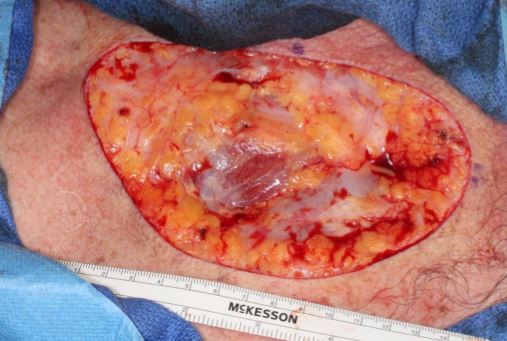
13.5 x 8.3 cm wide local excision defect of the upper chest.
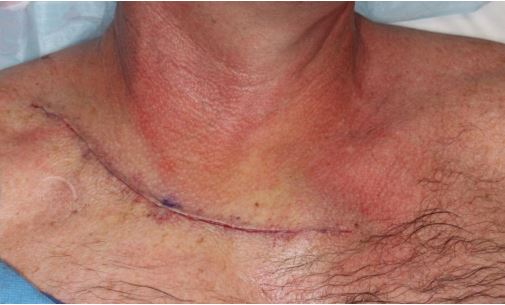
Immediate post-operative closure.
DISCUSSION
Very large basal cell carcinomas can be treated surgically with either Mohs excision or wide local excision (WLE) with permanent histology. At the SCARS Center, larger tumors are preferentially treated with wide local excision. WLE affords the opportunity for IV sedation anesthesia in the operating room setting and greater patient comfort. It decreases the amount of local anesthetic infiltration and its associated cardiovascular epinephrine effects. It also decreases the time the patient spends in the healthcare setting. Mohs excision of large cancers also creates a challenge for margin management and requires an extensive amount of slide review. As such, large tumors are associated with higher rate of post-Mohs recurrence.
WLE poses a risk for resection margin involvement which would require an additional procedure. However, most of these tumors have visually identifiable margins that can be treated with minimal margin of resection. In our case, it was 1 cm.
Perineural invasion (PNI) by basal cell carcinoma is not an uncommon finding. It is associated with larger and more aggressive basal cell carcinomas. PNI’s less aggressive cousin, perineural inflammation, is much more common and is also associated with larger tumors.
Adjuvant therapy must be considered with this type of tumor. Given the elevated risk of recurrence, post-operative radiotherapy is an option. In this patient, office based SRT is not possible due to the size of the area requiring treatment. Large machines with larger SSD (source to surface distance) limit the penumbra effect while delivering the large area of treatment.
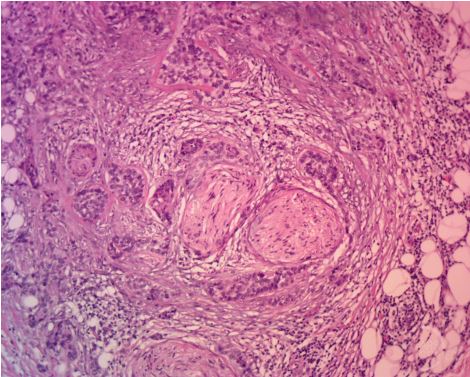
BCC PNI of chest.
