Nasal Open Wound Complication
HISTORY
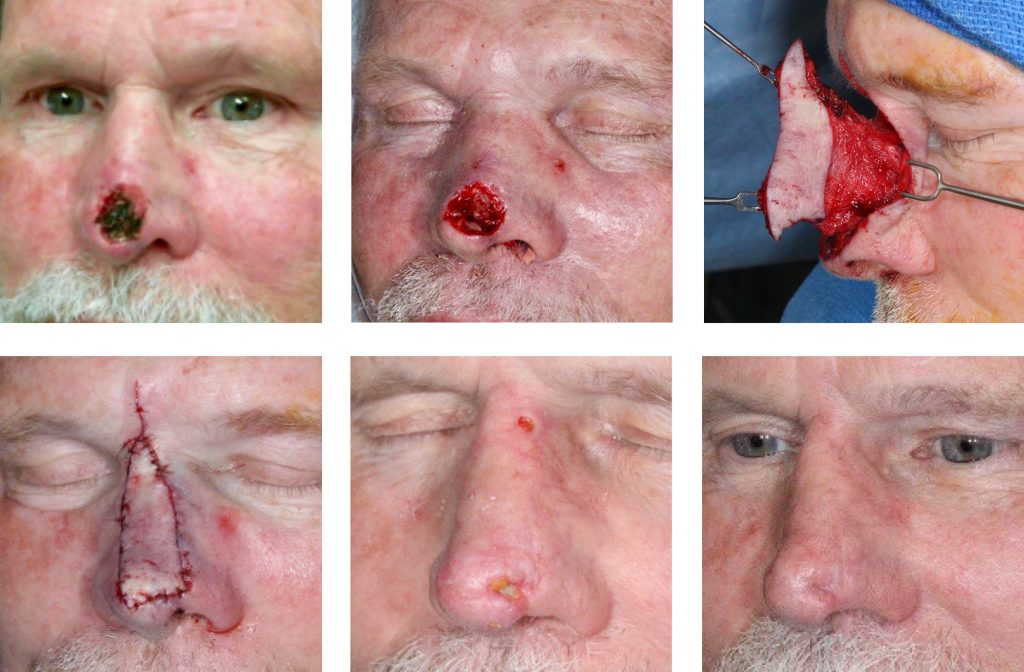
A 73-year-old man with BCC of the nasal tip presented 1 week following Mohs excision. His reconstruction was delayed for an additional week for a cardiac work up. Nasal reconstruction was performed with a superior extended nasal myocutaneous flap (SENMI flap) and nasal septal cartilage grafts. The patient developed nasal tip incisional discharge 1 week post-op and was treated with doxycycline. The wound was debrided 3 weeks post-op with finding of ischemic cartilage. The depressed scar was revised 7 weeks postoperatively with ear cartilage grafts.
DISCUSSION
Delayed reconstruction following Mohs excision is a common occurrence. Some brief delays for 1-2 days are planned in order to coordinate scheduling of Mohs excision and reconstructive surgery. Other delays are due to an underestimation of the Mohs defect and the Mohs surgeon’s ability to reconstruct the defect. The resultant referral to a plastic surgeon invariably delays open wound closure. The open wounds awaiting reconstruction need special considerations.
On the one hand, an open wound left to heal on its own can successfully achieve full secondary intention healing over 4-8 weeks. In some scenarios, a number of complications of open wounds are worth considering.
Contraction of the wound in certain anatomic locations can irreversibly alter the adjacent uninjured tissue. The nasal tip and ala defects will contract, irreversibly shrinking the internal lining of the nasal vestibule and mucosa. Subsequent reconstruction will require robust expansion of the internal lining. In these cases, the delay of wound closure changes a single layer skin reconstruction into a three layered complex reconstruction. Alternatively, acceptance of alar rim retraction with limited reconstruction will be required.
Other sites where contraction will change the reconstructive plan are eyelid defects near the lid margin and ear defects of the helix and scapha. Wound contraction begins around 10 days and completes by 4 weeks. Therefore, reconstruction must be performed within 2 weeks of open wound creation. After 4 weeks, the urgency to reconstruct wanes, and waiting for secondary intention healing to complete is reasonable.
A less common complication of an open wound is exposure of cartilage and its necrosis. Such is the case presented above. Alar cartilage and ear cartilage are at risk of exposure necrosis. When covered with soft tissue reconstruction, the infected dead cartilage forms a draining sinus tract. Its debridement and subsequent cartilage grafting is required to correct the scar.
Infection of the open wound is uncommon in most cutaneous wounds created by Mohs surgery. Exceptions are wounds of lower extremities and hands. Special consideration in immunocompromised, diabetic, and frail patients are also required.
Solutions to avoid complications of open wounds should primarily be based on good planning. Conservatively predicting the resultant Mohs defect is a must. In our center’s experience, the size of the Mohs defect can be predicted within a few millimeters in vast majority of cases. Discussion with the patient about the reconstruction can then take place. If plastic surgery involvement is required, a consultation and work-up coordination occurs prior to Mohs surgery.
In some cases, the extent of pathology is hard to ascertain. In these cases, we perform mapping biopsies of the lesion prior to Mohs excision. This is especially important in melanoma in situ, morpheaform cancers, and high risk cancers such as microcystic adnexal carcinoma and DFSP.
When the impending delay of open wound closure becomes apparent, temporary closure can avoid some complications. The simplest is closure with a porcine xenograft. Inexpensive off-the-shelf options are Mediskin and E-Z Derm. Xenografts avoid tissue desiccation, provide a barrier for contamination, and limit bleeding and oozing. Wound contraction is not avoidable with xenografts or even skin grafts.
