Sentinel Lymph Node Biopsy for Cutaneous SCC
HISTORY
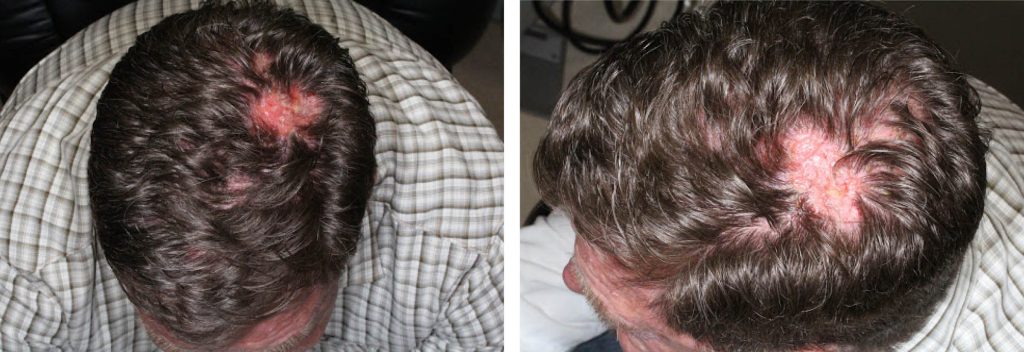
A 58-year-old kidney transplant recipient presented with a 6-month history of squamous cell carcinoma of the left scalp. This large lesion was adjacent to the scar of a previous carcinoma excision in 2014. Patient is on sirolimus for his kidney transplant performed in 1984. He has had multiple BCCs and SCCs of scalp, back, and nose. PET/CT scan found no evidence of metastases. Sentinel lymph node biopsy at the time of Mohs excision found no metastatic disease.
DISCUSSION
The role of sentinel lymph node biopsy (SLN bx) for cutaneous squamous cell carcinoma has been unclear. The indications for SLN bx are based on the risk factors of recurrence and metastases of SCC summarized in the NCCN guidelines. The high risk SCC factors particularly for metastases include perineural invasion, angiolymphatic invasion, and depth (> 4-6 mm, invasion into fat or muscle). Other risk factors include aggressive histologic subtype (adenoid, metaplastic, desmoplastic), size > 2cm, immunosuppression, and locally recurrent carcinoma. These latter risk factors are more associated with local recurrence risk. However, when multiple risk factors are present, they can predict metastatic risk as well.
Studies evaluating nodal involvement find that 12-15% of patients with above tumor criteria had metastases in their sentinel lymph nodes.
https://jamanetwork.com/journals/jamaotolaryngology/article-abstract/2533538
https://onlinelibrary.wiley.com/doi/abs/10.1002/hed.24120
https://journals.sagepub.com/doi/abs/10.1177/0194599813511949
Generally, at >10% risk of lymph node involvement, sentinel lymph node biopsy is offered to the patient. If positive lymph node is found, then regional lymphatic treatment is indicated. The treatment may include lymphadenectomy or radiation of the lymph node basin or both.
The rationale for sentinel lymph node biopsy in melanoma has been studied more extensively. The effect of SLN bx on patient outcome has been called into question. (Bigby et al, J Am Acad Dermatol 2019;80:1168-71) With melanoma, sentinel lymph node biopsies have been shown to have prognostic value but not improvement in outcome, when compared with observation and treatment of clinically obvious lymphadenopathy.
Those studies do not exist for cutaneous SCC. But the nature of regionally metastatic squamous cell carcinoma is different from regionally metastatic melanoma. So, the theory is that stopping SCC within the regional lymph node basin improves patient outcome. We are still waiting for the definitive study to prove this assertion.
Finally, histologic evaluation of sentinel lymph nodes must involve more than a cursory evaluation of H&E staining. Immunohistochemistry can increase sensitivity of micrometastases detection.
