LEFT FOREHEAD SQUAMOUS CELL CARCINOMA
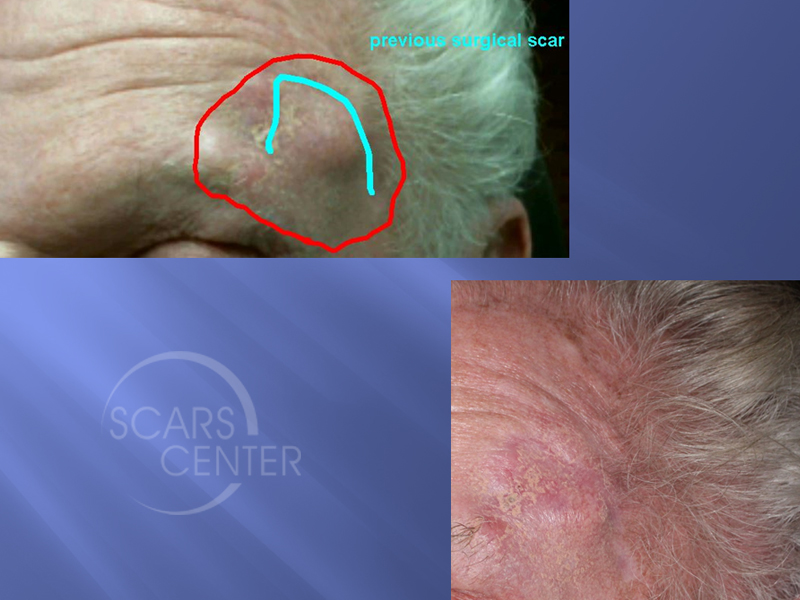
HISTORY
82 year old man presented in 02/2017 with a 3 year history of a crusty forehead lesion treated with cryoablation and 5-FU. Incisional biopsy in 2016 revealed poorly differentiated sclerosing squamous cell carcinoma, with perineural invasion. Excision a few months later was performed with residual circumferentially involved margins. CT with contrast showed only local tumor induration. CT/PET scan was negative.
DISCUSSION
This is an 82-year-old gentleman, who presented with a recurrent squamous cell carcinoma of the left forehead that was found to have perineural invasion. This is a highly aggressive tumor, initially presenting with a nodule that was subcutaneous in nature and subsequently undergoing a resection of frozen sections. This resection performed elsewhere found positive margins in all the aspects of frozen sections, which prompted the surgeon at that time to do an additional margin resection with immediate closure. All of those margins were found to be positive as well. The patient was recommended radiation therapy and while he waited, he developed additional lesions at the edge of the surgical reconstruction. The lowest portion of patient’s recurrence was on the supraorbital rim.
The most telling aspect of this patient’s case is the perineural invasion and the fact that nerves as large as 0.1 mm were involved with squamous cell carcinoma. The perineural involvement of nerves of 0.1 mm diameter or greater is a harbinger of potential lymphatic metastasis. Perineural invasion is associated with spread along nerves up to 2 cm from the gross tumor. If the patient’s supraorbital rim is the furthest palpable nodule, we can expect that the perineural invasion along the nerve may spread for 2 cm into the orbit. Some studies have shown that perineural spread can go as far as 4 cm, but those are rare cases. Skip lesions along the nerve past that distance are likely not direct perineural spread but metastases along the vascular and lymphatic channels.
Clearly, treatment of the patient requires not just surgical removal, but radiation therapy for sterilization of the field. If 2 cm margin is the margin of surgical excision and potentially radiation, then orbital resection or radiation is required in this particular patient. Spread along the temporal nerve branches down into the infratemporal fossa is also possibility. As a result, the only definitive treatment for this patient that could be considered curative would be wide local resection with orbital exenteration. The latter would be done only to facilitate radiation of the orbit. It is not possible to selectively radiate the orbit, sparing the globe. Such attempts are associated with with keratitis, orbital inflammation, chronic eye pain, and eventually result in removal of the eye for symptom relief. As a result if radiation of orbit is considered, then orbital exenteration as the primary treatment is the only reasonable course.
In this patient given the width of the cancer spread, resection of the entire forehead temple and orbit would be required followed by reconstruction with a free flap. Of course, acceptance by the patient of this radical approach is difficult. However, the conclusion of the SCARS Center multi-disciplinary conference was that anything short of the radical approach will result in cancer recurrence.
Work-up of this patient included a CT scan of the orbit as well as a CT/PET scan. Not surprisingly CT/PET scan did not find any positive findings in the lymphatics, in the orbit or in the primary tumor bed. We must remember that in order for CT/PET scan to actually enhance a lesion, a 4 mm nodule of hypermetabolic cancer must be present. Thin cancers would not light up in a CT/PET scan. Certainly microscopic spread along the nerves would never light up in a CT/PET scan given the modern resolution of these scans. Work-up of this patient could also include MRI of the orbit, which is also unlikely to show any sort of nerve involvement. MRI scans find supraorbital nerve involvement only if there is a palpable thickening of the nerve that is obvious. MRI in this patient will likely be noncontributory, but is worthwhile to check. It may find orbital apex nerve enlargement consistent with perineural invasion and spread.


