Sensory Symptoms with Skin Cancers
HISTORY
A 68-year-old woman presented with left cheek radiating, shooting pains in the area of biopsy proven basal cell carcinoma. The neuralgia symptoms radiated to the nose, eye, and temple. MRI of the face was non-contributory. Mohs excision was performed by the dermatologist. Additional margin wide local excision was performed at the reconstructive procedure. Patient continued to complain of left infraorbital paresthesia and neuralgia after surgery. Additional margin resection was negative for cancer.
DISCUSSION
Abnormal sensory symptoms associated with skin cancers can be a sign of deeper invasion, perineural invasion, and in transit metastases. There are two types of dysesthesia (sensory aberrations) associated with cutaneous carcinomas – symptoms of local uncomplicated cancer growth and symptoms of deeper infiltration with perineural invasion.
The most benign is patient awareness of early skin cancer growth. Some patients can reliably predict their skin cancers in the subclinical stage – before the cancer can be detected. Most commonly this presents as a local sensitivity to rubbing and touching.
Deeply invasive skin cancer can present with neuralgias – abnormal brief nerve symptoms such as shooting pains. These are manifestations of deeper direct invasion of sensory nerves. Great auricular nerve branches, trigeminal nerve branches (supraorbital, infraorbital, and mental nerves), and auriculotemporal nerves are susceptible to direct invasion. These nerves are superficial and, thus, most commonly affected.
The most ominous concern with neuralgia in the setting of a skin cancer is perineural invasion (PNI). Perineural invasion can present with sensory symptoms further away from direct cancer invasion. Example of such high risk presentations is a lower lip carcinoma with mental nerve neuralgia. One of the most dramatic cases I have seen involved forehead or temple squamous cell carcinomas with subtle periorbital neuralgias. These patients presented within a couple of months with periorbital, intraorbital, and intracranial metastases.
Patients presenting with neuralgias associated with skin cancer should be worked up with imaging. Ultrasound can reliably determine deeper cancer spread in the parotid gland and neck where palpation can be limited by the depth of cancer involvement. MRI is particularly useful for the orbit, infratemporal fossa, and brain. CT is highly sensitive for bone erosion by cancers in the inferior mandibular canal and the mental nerve.
If no gross tumor is found on imaging, the surgical management still needs to be planned with expectation of more extensive tumor spread. Mohs surgery should be planned with the back-up of an oncologic surgeon. Mohs guided wide local resection may need to be done. Patients may need to be prepared for larger reconstruction. Discussion of post-operative radiation therapy needs to occur with the patient. It has been found that evidence of microscopic nerve invasion of nerve diameter 0.1 mm or more is associated with lymphatic metastases.
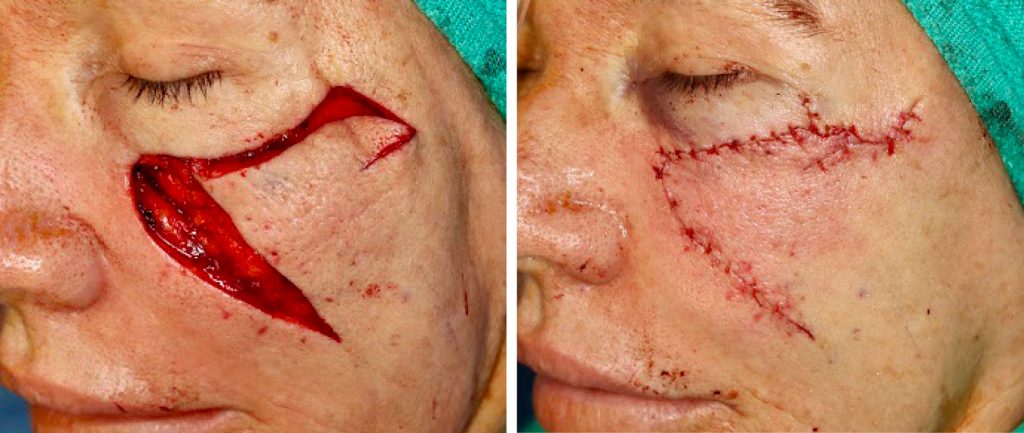
In our case, despite negative MRI and clear Mohs margins, a deeper soft tissue level was resected and submitted as FFPE histology at the time of reconstruction. Fortunately, no additional deeper cancer was found. This has been reassuring given that the patient continued to complain of infraorbital neuralgias. These were attributed to direct surgical injury and watchful waiting was the plan.